📌 Key Takeaways:
- No single diet permanently “resets” metabolism; improvements come from consistent calorie balance, nutrient-dense eating, and lifestyle factors that enhance metabolic flexibility.
- Mediterranean-style or DASH patterns with higher protein (1.2–1.6 g/kg), fiber (>30 g/day), and regular activity improve insulin sensitivity and cardiometabolic markers.
- Rapid restrictive approaches risk metabolic slowdown and regain; prioritize gradual, evidence-supported changes for sustainable results.
Introduction
Metabolic health issues, including insulin resistance, elevated blood glucose, and abdominal obesity, affect hundreds of millions worldwide and raise risks for type 2 diabetes, cardiovascular disease, and fatigue. In 2026, lifestyle-related metabolic dysfunction remains a leading concern amid processed food availability and sedentary patterns.
Clinical authorities emphasize that metabolic function improves through modifiable habits rather than quick fixes. This guide targets adults seeking better energy, body composition, and disease prevention. Readers receive actionable, guideline-aligned strategies: optimizing meals for macronutrients and fiber, incorporating movement, prioritizing recovery, and monitoring progress realistically. Expect gradual enhancements in how the body switches between fuel sources (metabolic flexibility) and manages energy when habits align consistently.
What Metabolic Health and Flexibility Actually Mean
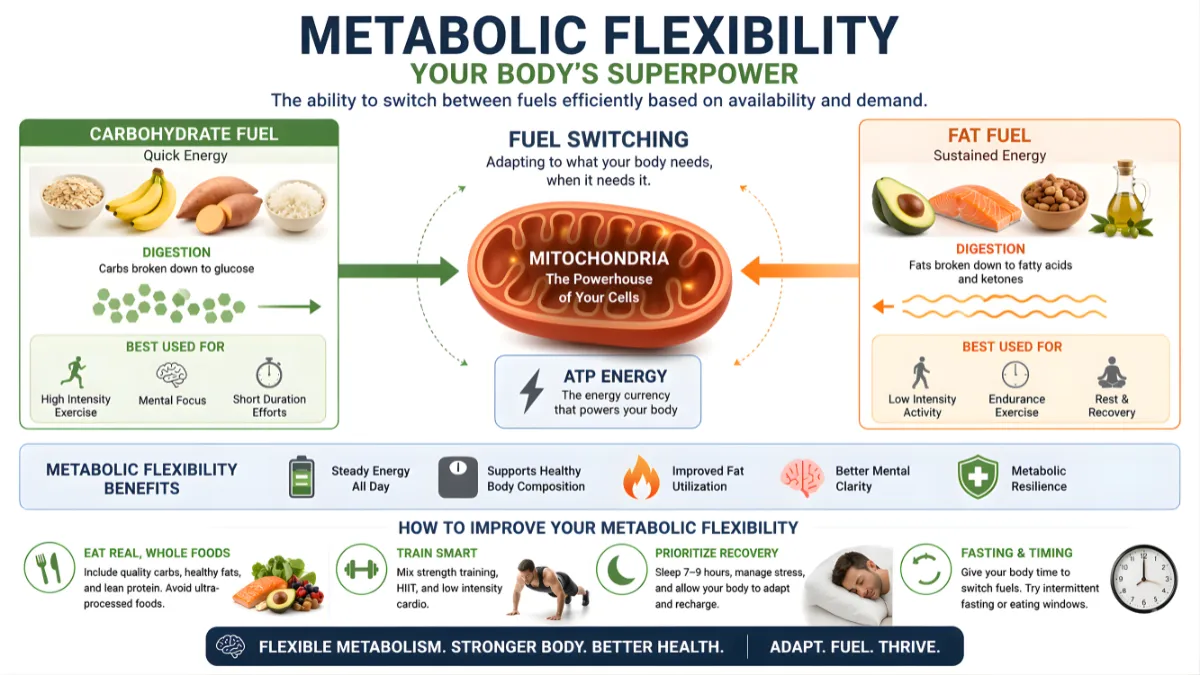
Metabolic flexibility describes the body’s ability to efficiently switch between burning carbohydrates (fed state) and fats (fasted or active state). Reduced flexibility links to insulin resistance and fat storage. Evidence shows lifestyle interventions restore aspects of this adaptability without extreme measures.
Key influencers include diet composition, physical activity, sleep, and stress. Short-term calorie restriction or fasting can temporarily shift fuel use, but long-term gains require ongoing habits. Systematic reviews confirm that weight loss of 5–10% and sustained healthy eating patterns yield measurable improvements in glucose control, lipids, and inflammation.
Practical Signs of Progress:
- More stable energy between meals
- Improved fasting blood glucose or HbA1c (if monitored)
- Easier fat loss or maintenance with moderate calories
- Better recovery from exercise
Core Dietary Principles for Metabolic Improvement
Focus on nutrient-dense, minimally processed foods that support stable blood sugar and satiety. Prioritize patterns like Mediterranean or DASH, which reduce metabolic syndrome components.
Macronutrient Guidance (for ~1,800–2,200 kcal example, adjust per needs):
- Protein: 1.2–1.6 g/kg body weight (e.g., 90–130 g for 75 kg person) for muscle preservation and satiety.
- Carbohydrates: 45–55% from fiber-rich whole sources.
- Fats: 25–35%, emphasizing unsaturated (olive oil, nuts, fatty fish).
- Fiber: Aim for 30–40 g/day from vegetables, fruits, legumes, and whole grains.
Sample Daily Meal Framework (~1,900 kcal):
- Breakfast: Oatmeal (50 g) with berries (150 g), Greek yogurt (150 g), and almonds (20 g) — high fiber, ~25 g protein.
- Lunch: Grilled salmon (120 g), quinoa (60 g cooked), large mixed salad with olive oil, chickpeas (80 g) — balanced macros.
- Dinner: Lentil stew with vegetables, spinach, and lean chicken or tofu (120 g) plus sweet potato.
- Snacks: Apple with handful of walnuts or carrot sticks with hummus.
Emphasize meal timing with 10–12 hour eating windows for many, allowing natural fasting periods without extremes.
Exercise and Movement Strategies
Physical activity ranks among the strongest tools for metabolic health. Combine aerobic and resistance work to improve insulin sensitivity and mitochondrial function.
Recommended Weekly Structure:
- 150+ minutes moderate aerobic (brisk walking, cycling).
- 2–3 resistance sessions (full body: squats, rows, presses) to build/preserve muscle.
- Daily NEAT: Aim for 7,000–10,000 steps.
Resistance training particularly enhances glucose uptake in muscles. HIIT or interval work offers efficient benefits for time-constrained individuals.
Comparison Table: Activity Approaches for Metabolic Health
| Feature | Resistance Training | Steady-State Cardio | Combined Approach |
|---|---|---|---|
| Insulin Sensitivity | High | Moderate | Highest |
| Muscle/Fat Impact | Preserves/builds muscle | Modest fat loss | Optimal body composition |
| Weekly Time | 3 sessions (45 min) | 150+ min | Flexible 4–5 sessions |
| Long-Term Benefits | Metabolic rate support | Cardiovascular health | Comprehensive risk reduction |
| Best For | Beginners to advanced | Endurance focus | Most adults |
Sleep, Stress, and Behavioral Factors
Sleep deprivation impairs glucose tolerance and increases hunger hormones. Target 7–9 hours nightly with consistent schedules. Chronic stress elevates cortisol, promoting abdominal fat storage.
Incorporate mindfulness, walking, or breathing practices. Behavioral tracking (food, activity, sleep logs) supports adherence.
Risks and Contraindications: Very-low-calorie or prolonged extreme fasting can reduce metabolic rate and nutrient status. Avoid aggressive restriction if pregnant, underweight, or with eating disorder history. High-protein needs caution with advanced kidney disease. Consult healthcare providers for personalized plans, especially with medications or conditions.
Popular Patterns Comparison for Metabolic Support
Evidence-Based Comparison Table:
| Pattern | Key Focus | Metabolic Benefits | Sustainability | Limitations |
|---|---|---|---|---|
| Mediterranean | Plants, fish, olive oil, nuts | Improved insulin sensitivity, lipids | High | Requires meal planning |
| DASH | Fruits/veg, low sodium, dairy | Blood pressure & glucose control | High | Less emphasis on healthy fats |
| Higher-Protein/Flexible | Balanced + protein priority | Satiety, muscle retention | Moderate-High | Monitoring portions |
| Time-Restricted Eating | 10–12 hour window | Potential flexibility aid | Moderate | Social/adherence challenges |
Conclusion
Improving metabolic health involves nutrient-rich eating patterns, regular movement, quality sleep, and stress management rather than temporary resets. These evidence-based habits enhance flexibility, support healthy weight, and reduce disease risk over months to years. Next steps: Assess current habits for one week, adopt a Mediterranean-style plate (half vegetables, quarter protein, quarter whole grains), add two strength sessions, and prioritize sleep. Track energy and measurements over 4–8 weeks. Long-term perspective frames this as lifelong self-care yielding sustained vitality and prevention benefits. Work with a registered dietitian or clinician for tailoring, especially when addressing specific conditions. Consistency drives meaningful, lasting change.
FAQ — People Also Ask
Q: Can you really reset your metabolism with diet?
A: Metabolism adapts to habits but does not reset like a switch. Sustainable improvements occur through balanced nutrition, activity, and sleep.
Q: What foods improve metabolic health?
A: Prioritize vegetables, fruits, legumes, whole grains, lean proteins, nuts, and olive oil while limiting ultra-processed foods and added sugars.
Q: How long does it take to see metabolic improvements?
A: Noticeable changes in energy and labs often appear in 4–12 weeks with consistent habits; deeper benefits accumulate over months.
Q: Is intermittent fasting necessary for metabolic reset?
A: Not required. Moderate time-restricted eating (10–12 hours) may help some, but overall diet quality and calorie balance matter more.
Q: Who should avoid aggressive metabolic diets?
A: Individuals with eating disorders, pregnancy, certain medical conditions, or on specific medications should consult providers first.
References
- https://www.medicalnewstoday.com/articles/metabolic-reset https://pmc.ncbi.nlm.nih.gov/articles/PMC12376428/ https://www.cdc.gov/obesity/php/about/consequences.html
- https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight https://pubmed.ncbi.nlm.nih.gov/31899037/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8308821/
- https://www.health.harvard.edu/blog/exercise-metabolism-and-weight-new-research-from-the-biggest-loser-202201272676